Home » Cancer Types » Pediatric Oncology
Pediatric Oncology
- Overview
- Treatment Options
- What to Expect
Pediatric cancers consist of a wide variety of tumors arising in children involving nearly every organ of the body. Over 50% of the 9,800 cases of childhood cancers diagnosed each year in the United States are leukemias or brain tumors. Other pediatric cancers include Hodgkin’s lymphoma, Wilm’s tumor, Ewing’s sarcoma, rhabdomyosarcoma, neuroblastoma, and retinoblastoma. Many of these tumors are extremely uncommon.
ROA has been the primary radiation treatment center for the pediatric population in Northern Virginia for over a decade. ROA is the largest radiation oncology practice in the Washington, D.C. area. We are large enough that our doctors are specialized with expertise in particular cancer types, treatments, and even ages. Dr. Avani Rao, Dr. Samir Kanani, Dr. Kevin Choe, and Dr. Michael Eblan lead our team of specialists who work closely with the pediatric teams at National Children’s Medical Center and Inova Fairfax Hospital for Children to provide the highest quality radiation treatment for our pediatric patients. Through participation in multidisciplinary clinics and tumor boards with pediatric oncologists, surgeons, radiologists, pathologists, and neurocognitive experts, our pediatric radiation program provides comprehensive care with consideration and input from all of the important pediatric specialties before each recommendation is made. Dr. Rao, Dr. Kanani, Dr. Choe and Dr. Eblan are members of the Children’s Oncology Group (COG) and we offer radiation treatment on all of their pediatric cancer protocols.
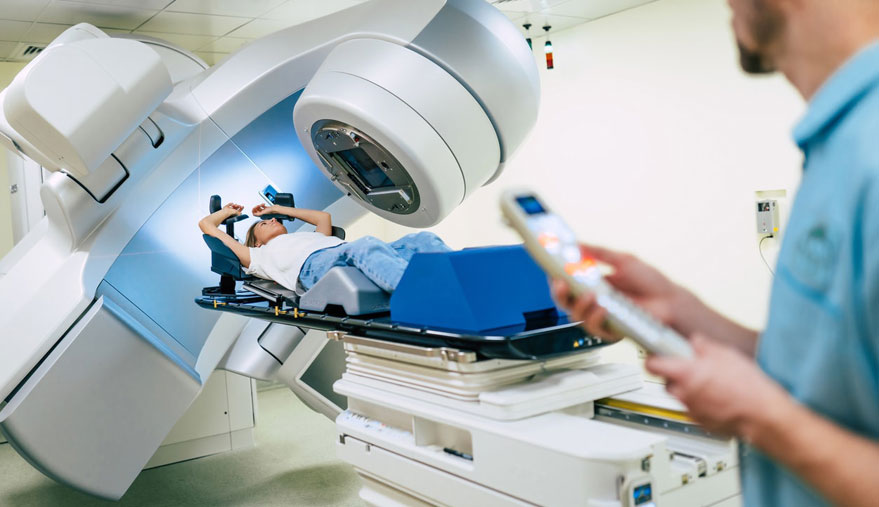
Radiation therapy has always maintained an important role in the treatment of childhood cancers. In the past, pediatric patients were treated with large radiation fields and relatively high doses of radiation to achieve long-term cures. Over time we have gained an appreciation of the long-term effects of radiation in the pediatric population. Today we take every step to minimize the radiation exposure of our young patients. The increasing use of chemotherapy and substantial improvements in the accuracy of radiation treatment have enabled radiation oncologists to dramatically reduce the amount of radiation necessary to cure our patients. At the same time, because of these novel approaches the long-term effects of radiation on our patients are expected to be significantly lower. At ROA, we are keenly aware of this emerging concept in pediatric oncology and carefully consider this for every patient and family we see in consultation.
A wide variety of radiotherapy techniques are currently used in childhood cancers. In some childhood cancers it is necessary to treat a large area because there is a risk for cancer involvement throughout. In this setting conventional radiation techniques are used which intentionally do not block normal tissues. A classic example of this is the central nervous system where cancer cells may have access to the entire circulation of cerebrospinal fluid that surrounds the brain and spinal cord, and this compartment must be treated in its entirety to ensure that all cancer cells are destroyed. In contrast, some cancers require high dose treatment to a small, localized target that may be located in close proximity to critical and/or sensitive normal tissues. In this case highly technical radiation delivery is indicated to deliver the needed dose to the tumor while minimizing any collateral radiation to the surrounding normal tissues. ROA is proud to offer numerous options for these patients including:
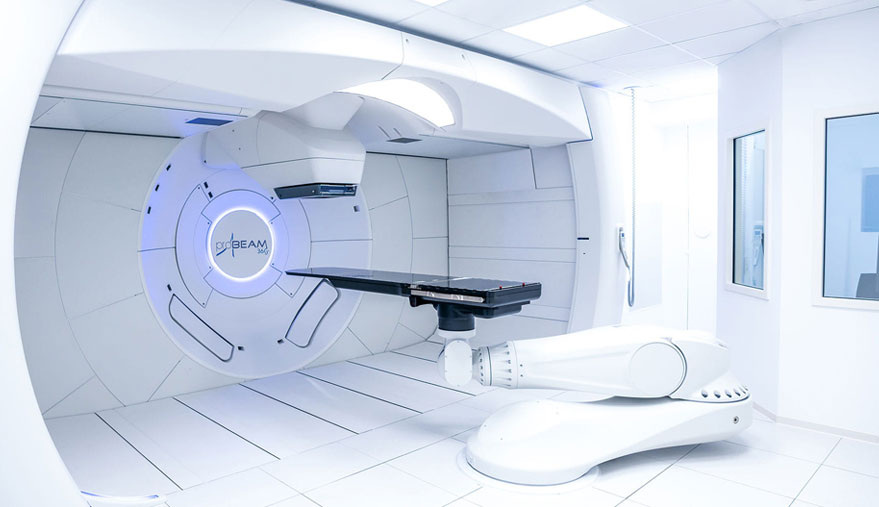
- Proton Therapy
- 3D Conformal Radiation Therapy
- Intensity-Modulated Radiation Therapy
- Stereotactic Radiosurgery (SRS) (See also Frameless SRS)
- Stereotactic Body Radiation Therapy (SBRT)
- Image-Guided Radiation Therapy (IGRT)
- Respiratory-Gated Radiation Therapy (RGRT)
- Pediatric Anesthesis
We the first in the area to offer Proton Beam Radiotherapy, which is a highly advanced form of radiation treatment that precisely targets a tumor, while sparing healthy tissues and organs from the damaging side-effects of radiation. Additionally, we also offer Intensity-Modulated Radiation Therapy (IMRT), Stereotactic Radiosurgery (SRS), Stereotactic Body Radiation Therapy (SBRT), Image-Guided Radiation Therapy (IGRT), or some combination of these highly technical radiation treatments.
Your radiation oncologist considers the advantages of every treatment device and technique when deciding on the optimal treatment approach for each patient. After an initial consultation with the doctor, it may be determined that your child will require anesthesia during radiation treatment. This is often the case for pediatric patients under the age of 4, but this decision is always made on an individual basis. Our dedicated staff is highly experienced with the treatment of children under anesthesia. The Radiation Oncology Department works closely with the Department of Anesthesia to ensure that both the radiotherapy and anesthesia are administered safely and effectively.
Effective, safe and compassionate patient care is our top priority
Your radiation oncologist will work with your child’s oncology team to determine the most appropriate treatment option for your child. Under most circumstances, your child will need to be treated with a number of modalities including surgery, chemotherapy, targeted therapy and radiation.
Effective, safe and compassionate patient care is our top priority
Latest News
Dr. Lonika Majithia publishes on The Clinical Utility of DCISionRT on Radiation Therapy Decision Making in Patients with Ductal Carcinoma In Situ Following Breast-Conserving Surgery in Annals of Surgical Oncology
Abstract Background The role of radiation therapy (RT) following breast-conserving surgery (BCS) in ductal carcinoma in situ (DCIS) remains controversial. Trials have not identified a low-risk cohort, based on clinicopathologic features, who do not benefit from RT. A biosignature (DCISionRT®) that evaluates recurrence risk has been developed and validated. We evaluated the impact of DCISionRT […]
Dr. Avani Rao publishes on plan quality effects of proton therapy for central nervous system and skull base tumors in Radiotherapy and Oncology
Abstract Purpose With reports of CNS toxicity in patients treated with proton therapy at doses lower than would be expected based on photon data, it has been proposed that heavy monitor unit (MU) weighting of pencil beam scanning (PBS) proton therapy spots may potentially increase the risk of toxicity. We evaluated the impact of maximum […]
Dr. Daniel Kim publishes on the implications of practice consolidation among radiation oncologists
Abstract Purpose Health care practices across the United States have been consolidating in response to various market forces. The degree of practice consolidation varies widely across specialties but has not been well studied within radiation oncology. This study used Medicare data to characterize the extent of practice consolidation among radiation oncologists and to investigate associated […]
Cancer Types
Radiation Oncology Associates is the leader in comprehensive and cutting-edge radiation oncology therapy services in convenient and accessible locations across Northern Virginia.